Training During Perimenopause
Training during perimenopause often feels more challenging—not because the body loses its ability to adapt, but because the conditions that support adaptation become less consistent.
Hormonal fluctuations, combined with increasing life stress, change how the body responds to training. The goal isn’t to train less—it’s to train more intentionally.
Training Capacity Changes — Not Potential
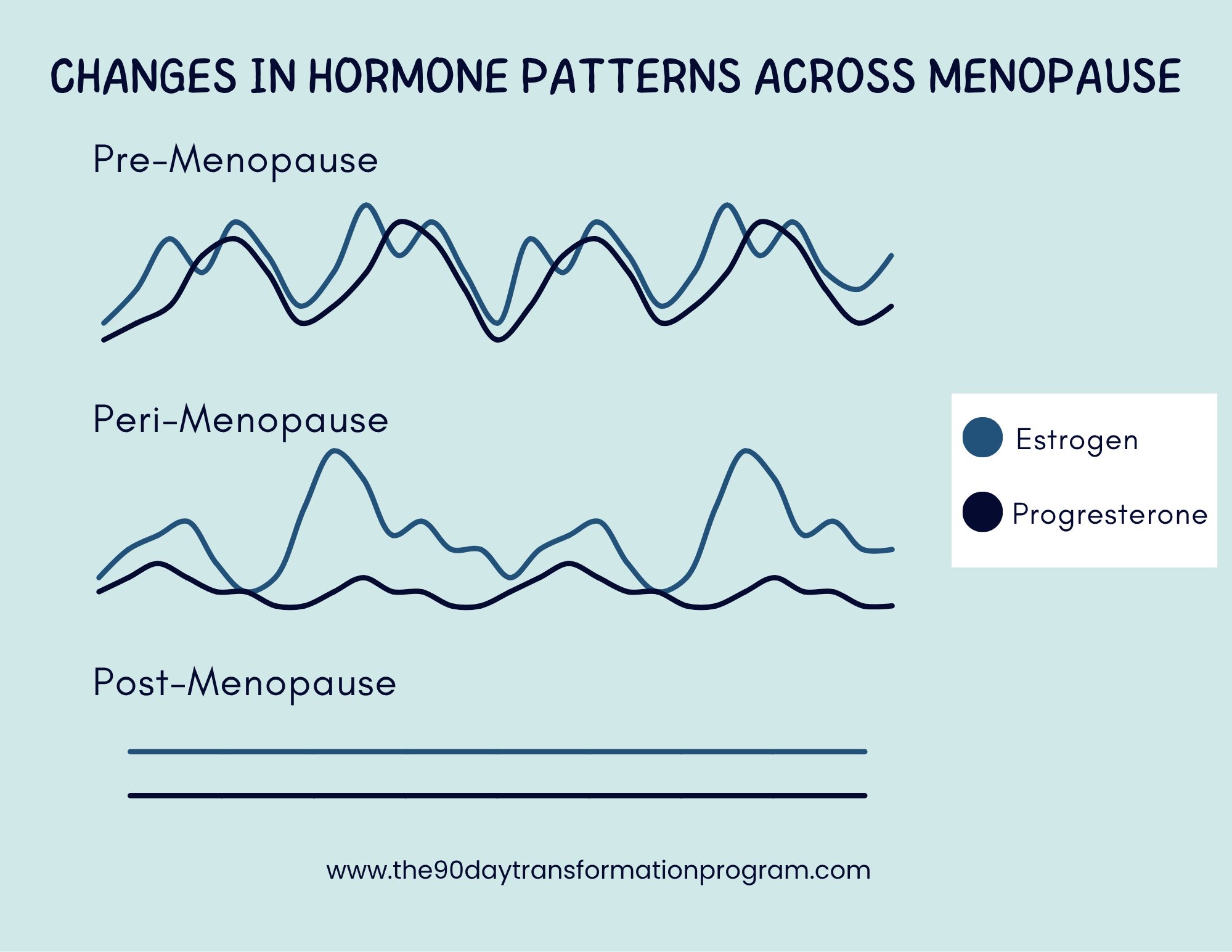
Perimenopause is characterized by variability in estrogen and progesterone.
Estrogen influences muscle repair, glucose regulation, and connective tissue health. Progesterone affects nervous system regulation and perceived effort. As these hormones fluctuate, recovery speed, fatigue, and training tolerance can vary from week to week.
This is why the same workout that once felt manageable may now feel significantly harder to recover from.
Recovery Becomes the Limiting Factor
Research and practical observation both show that during this phase, the body becomes more sensitive to total stress load.
Training stress doesn’t exist in isolation—it interacts with:
Sleep quality
Work and life stress
Nutrition
Hormonal variability
When recovery isn’t sufficient, this can show up as:
Persistent soreness
Reduced performance
Increased injury risk
Stalled progress despite effort
The issue isn’t effort—it’s recoverability.
Strength Training Becomes Foundational
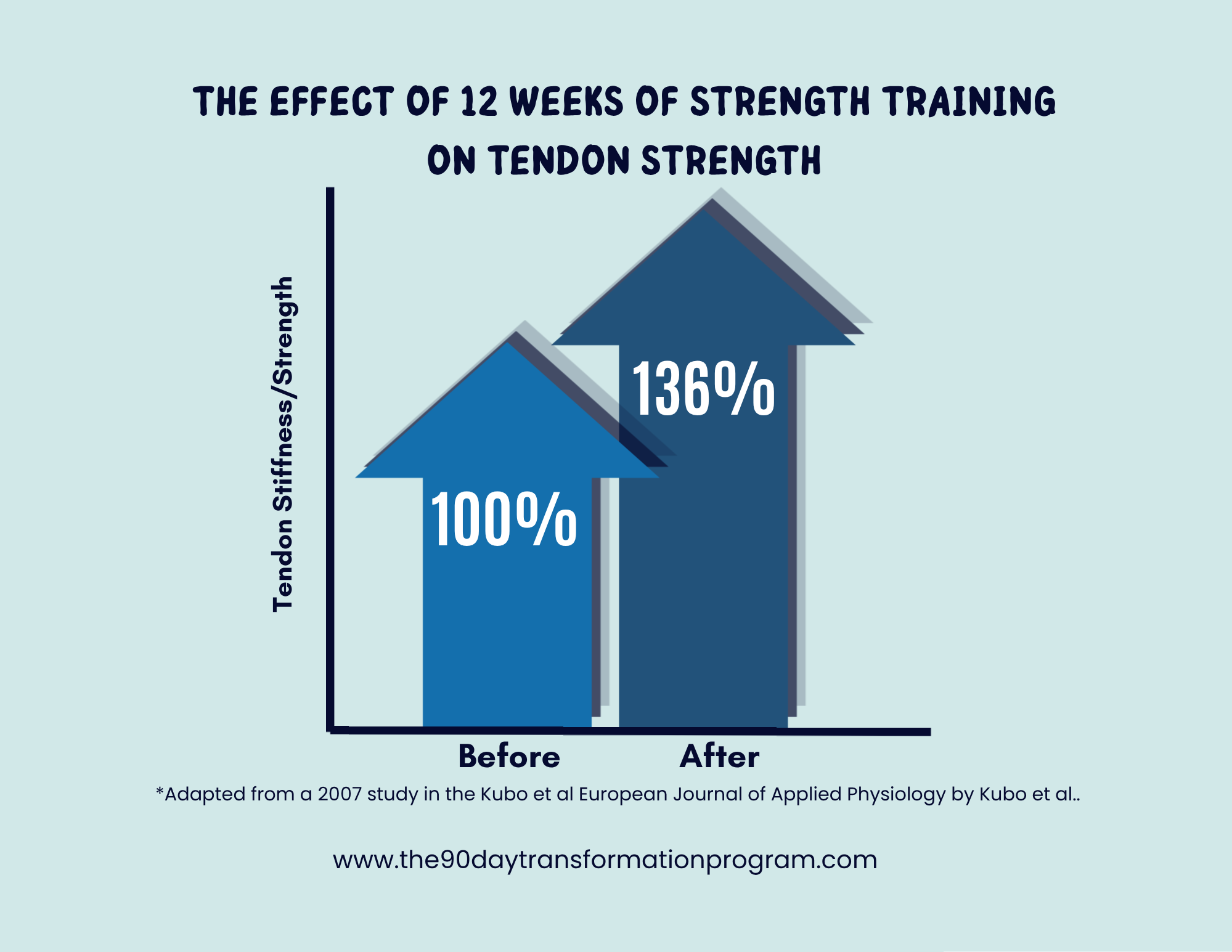
Resistance training remains the most effective anchor during perimenopause.
It provides a consistent mechanical stimulus that supports:
Muscle preservation
Bone density
Metabolic health
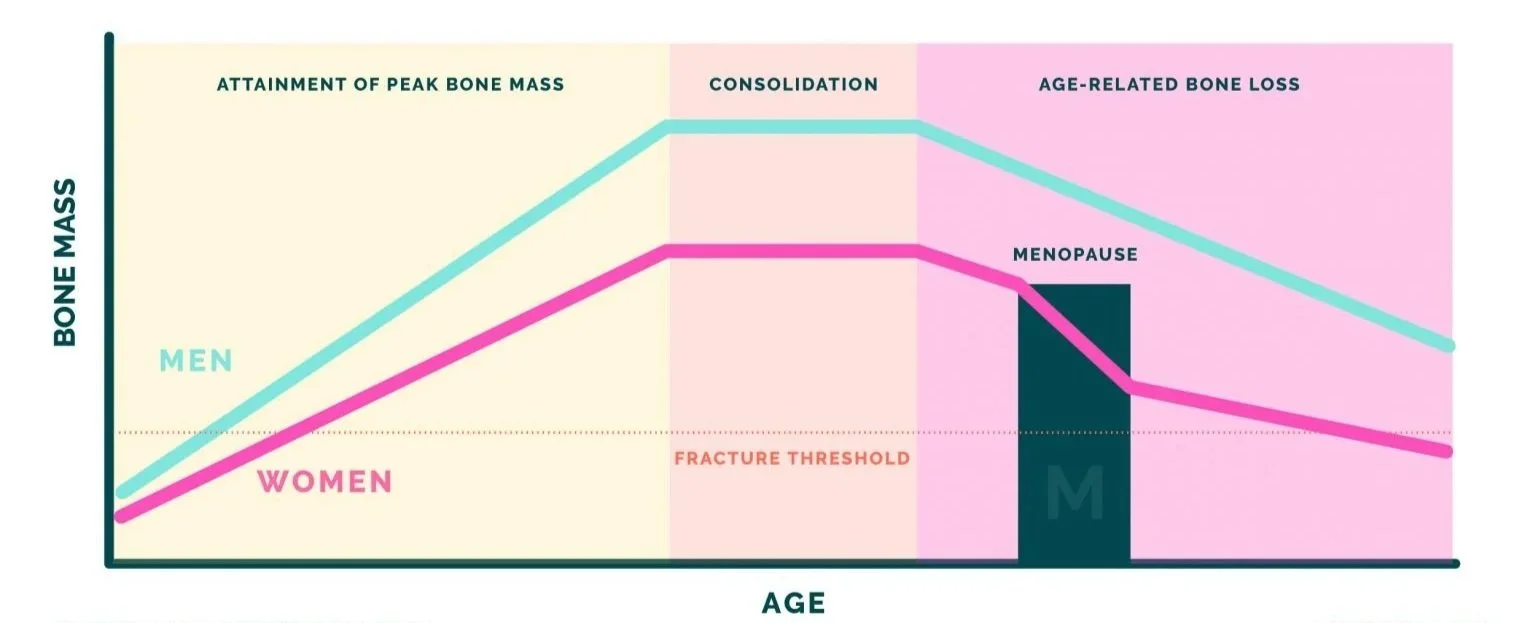
This graph from the Journal of Clinical Endocrinology shows how bone mineral density is affected by age, gender and peri-menopause.
Unlike fat loss strategies or high-volume training, strength training is reliable even when hormones are not.
Volume Often Needs Refinement
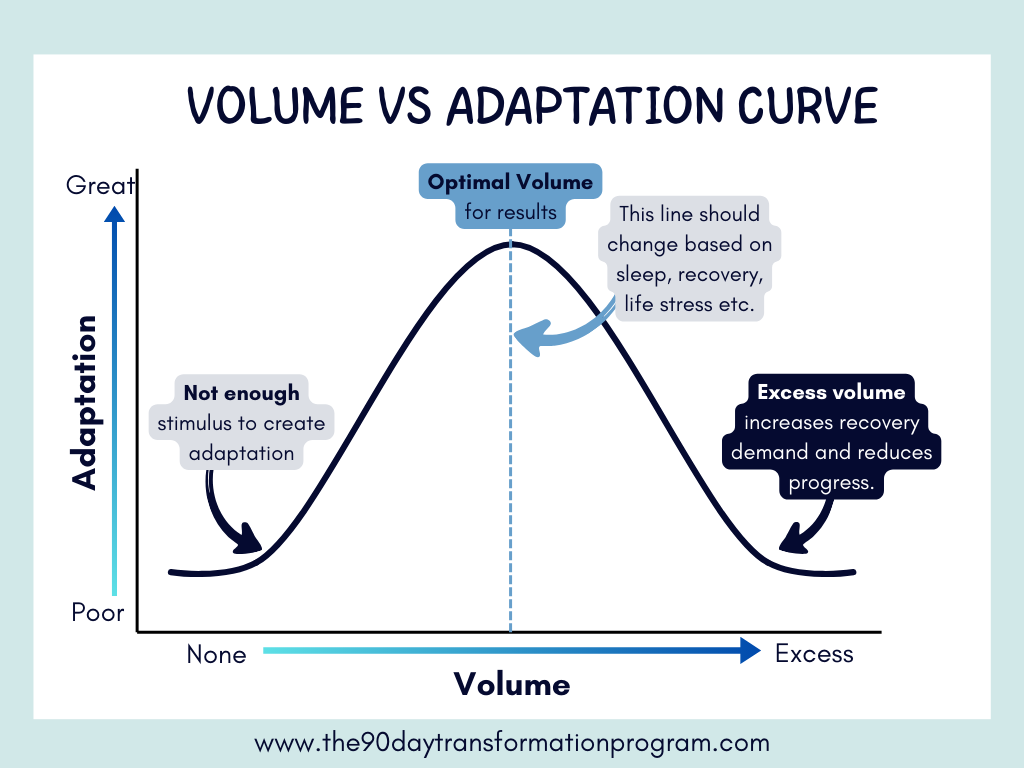
More is not always better—especially during this phase.
High training volume increases recovery demands and can exceed what the body can adapt to consistently. This doesn’t mean reducing intensity, but rather moderating volume while maintaining quality.
Shifting the focus from “How much can I do?” to “What is the minimum effective dose?” often leads to better outcomes.
Conditioning Should Support, Not Compete
Cardio still has a place—but it needs to be used strategically.
Frequent high-intensity conditioning can:
Elevate stress hormone activity
Impair recovery
Interfere with strength adaptations
Lower-intensity work can support recovery and cardiovascular health when balanced appropriately.
The key is ensuring conditioning complements strength training—not competes with it.
Autoregulation Improves Consistency
Rigid programs often fail when the body becomes less predictable.
Autoregulation—adjusting training based on readiness—becomes a valuable tool.
This can be guided by:
Energy levels
Sleep quality
Perceived exertion
Rather than forcing consistency in output, the goal becomes consistency in showing up and adjusting appropriately.
Nutrition Drives Adaptation
Training results are heavily influenced by how well the body is fueled.
During perimenopause, adequate nutrition becomes even more important:
Protein supports muscle repair and preservation
Carbohydrates support training performance and stress regulation
Sufficient energy intake supports recovery capacity
Training in a chronically under-fueled state increases stress hormone activity and amplifies fatigue.
What previously “worked” nutritionally may no longer be enough.
In Summary
Training during perimenopause doesn’t require doing less—it requires doing what matters, more precisely.
Progress is best supported by:
Consistent strength training
Managed training volume
Strategic conditioning
Adequate fueling
Intentional recovery
Perimenopause isn’t a barrier to progress. It’s a shift in how the body responds.
When training aligns with that reality, women can continue to build strength, maintain muscle, and support long-term health—with less frustration and more consistency.